Excellus BCBS report shows one third of those seeking behavioral health services do so through telemedicine
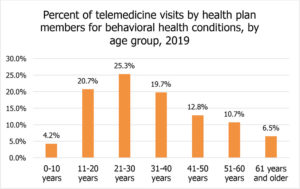 Behavioral health services delivered via telemedicine now accounts for nearly one-third of all telemedicine visits, according to a review of 2019 claims data by Excellus BlueCross BlueShield.
Behavioral health services delivered via telemedicine now accounts for nearly one-third of all telemedicine visits, according to a review of 2019 claims data by Excellus BlueCross BlueShield.
In 2018, behavioral health services accounted for less than 25% of all telemedicine visits. The health plan serves more than 1.5 million members across 39 counties of Upstate New York.
Telemedicine allows a health care provider to treat a patient by telephone or a secure, two-way video connection that is similar to Skype or FaceTime. Private insurance, Medicare and Medicaid pay for health care services delivered via telemedicine.
Behavioral health services include treatment for mental health conditions and substance use disorders. The top mental health conditions for which health plan members seek telemedicine treatment are generalized anxiety disorders, major depressive disorders, dysthymic disorders, posttraumatic stress disorders and adjustment disorders. The use of telemedicine for behavioral health services also includes treatment of substance use disorders including opioid use disorders, alcohol use disorders and tobacco use disorders. The top specialists seen via telemedicine for behavioral health treatment include social workers, psychologists, counselors and nurse practitioners.
“Patients are realizing that they can see a specific behavioral health provider on an ongoing basis from the privacy of their home, where they feel comfortable and can call at their convenience,” said Marya Vande-Doyle, director of workplace wellness and telemedicine for Excellus BlueCross BlueShield. “Another factor in many parts of upstate New York may be the shortage of behavioral health professionals, especially those who specialize in treating children and adolescents. Telemedicine can easily connect these patients with accessible behavioral health providers from whom they can receive ongoing care.”
Extrapolating the health plan’s member claims data to reflect the entire statewide population, Vande-Doyle estimates that New Yorkers logged more than 80,000 telemedicine visits for behavioral health services in 2019.
A survey of upstate New York adults conducted in late 2019 by One Research and commissioned by Excellus BlueCross BlueShield found that among 2,000 respondents:
• 17% are receiving counseling for a mental health condition,
• 28% are taking medication for a mental health condition,
• 35% say they will consider using telemedicine for treatment of a mental health condition,
• 58% of participants who said they take a medication or are receiving counseling for a mental health condition say they will consider using telemedicine to connect with a health care provider.
Using telemedicine to access behavioral health services is most popular among patients in younger age brackets. A review of health plan claims data found that approximately 70 percent of users are 40 years old or younger. About one-quarter of users are 20 years old or younger.
“Many of my clients are young working professionals and are not intimidated by the use of technology for our sessions,” said Tara Ammersen, Syracuse, a licensed clinical social worker who uses telemedicine to meet with patients. “Also, my clients with children appreciate that they don’t have to arrange for child care while away from home for a session.”
“Telemedicine for behavioral health services isn’t for everyone and every situation,” said Vande-Doyle. “The significant year-over-year increase in its use for behavioral health services clearly demonstrates its growing acceptance as a tool that enhances access to care.”